The HDL cholesterol test is a key test in checking heart health. It’s called “good” cholesterol because it cleans up the blood. It picks up extra cholesterol from artery walls and takes it to the liver for removal.
To check HDL levels, a simple blood test is needed. Doctors use a lipid panel to measure HDL. Patients must fast for 9 to 12 hours before the test. The results show how much protective cholesterol is in the blood, in milligrams per deciliter (mg/dL).
Knowing the HDL normal range is key to preventing heart attacks and strokes. The American Heart Association says adults should get their cholesterol checked every four to six years. Those with health issues might need to go more often.
The HDL range tells a lot about heart disease risk. HDL is a fatty substance in every cell. Low HDL levels make arteries more likely to get clogged, increasing heart disease risk.
Key Takeaways
- HDL cholesterol is known as “good” cholesterol because it removes harmful cholesterol from the arteries.
- The HDL normal range is measured in milligrams per deciliter (mg/dL) through a standard lipid panel blood test.
- Fasting for 9 to 12 hours before the test is necessary for accurate results.
- The American Heart Association recommends cholesterol screenings every four to six years for low-risk adults starting at age 20.
- Understanding HDL levels helps doctors evaluate a patient’s risk for heart attack and stroke.
- A healthy high-density lipoprotein range supports the body’s ability to clear excess cholesterol from blood vessels.
What the HDL Test Measures
An HDL cholesterol test checks the amount of high-density lipoprotein cholesterol in your blood. It’s a key part of a complete lipid panel. This panel also looks at LDL cholesterol, triglycerides, and very-low-density lipoproteins (VLDL). Knowing your HDL levels helps doctors check your heart health and disease risk.
Definition of HDL Cholesterol
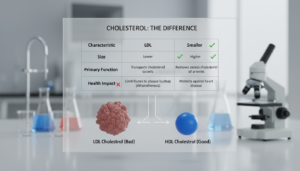
HDL stands for high-density lipoprotein. It’s a protein-fat particle that carries cholesterol. Known as “good” cholesterol, HDL removes excess cholesterol from artery walls and takes it to the liver. The liver then breaks it down and removes it from your body.
Total blood cholesterol is the sum of HDL and LDL cholesterol plus 20% of triglycerides, says the American Heart Association.
Importance of HDL in the Body
Healthy HDL cholesterol levels are key to heart health. HDL acts like a scavenger, removing harmful cholesterol from blood vessels. Without it, plaque builds up, causing atherosclerosis — a dangerous narrowing of arteries.
Key HDL functions include:
- Removing excess cholesterol from artery walls
- Transporting cholesterol to the liver for disposal
- Reducing inflammation in blood vessels
- Protecting against cell damage
Studies by the National Institutes of Health show that healthy HDL levels lower heart attack and stroke risks. Getting your HDL levels checked is the first step to spotting heart health issues.
Why the HDL Test is Ordered
Doctors order an HDL test for certain reasons related to a patient’s health. It’s part of a lipid panel that checks different types of cholesterol in the blood. By looking at HDL cholesterol guidelines, doctors can figure out how often to test patients and what actions to take based on the results.
Routine Health Screenings
Screening times vary based on age, family history, and risk factors. The American Heart Association suggests adults over 20 get tested every four to six years. Kids should have their first test between 9 and 11 years old, with tests every five years after that.
Some kids might need to be tested earlier, even at age 2, if they have a family history of high cholesterol or heart disease. Knowing the HDL range early helps families take steps to prevent problems.
“Screening for lipid disorders is one of the most effective strategies for early detection and prevention of cardiovascular disease.” — National Heart, Lung, and Blood Institute
| Age Group | Recommended First Test | Repeat Frequency |
|---|---|---|
| Children (no family risk) | Ages 9–11 | Every 5 years |
| Children (with family risk) | As early as age 2 | As directed by physician |
| Adults aged 20+ | Age 20 | Every 4–6 years |
| Adults with risk factors | Age 20 | Every 1–2 years |
Risk Assessment for Cardiovascular Disease
The HDL test is also important for checking cardiovascular risk. Doctors look at HDL levels, LDL, triglycerides, blood pressure, and blood sugar. This helps figure out a patient’s risk of heart disease or stroke over 10 years.
If HDL results are not in the optimal range, doctors might suggest lifestyle changes or medication. Following HDL cholesterol guidelines helps doctors create treatment plans that fit each patient’s risk.
Normal Reference Range for HDL Cholesterol
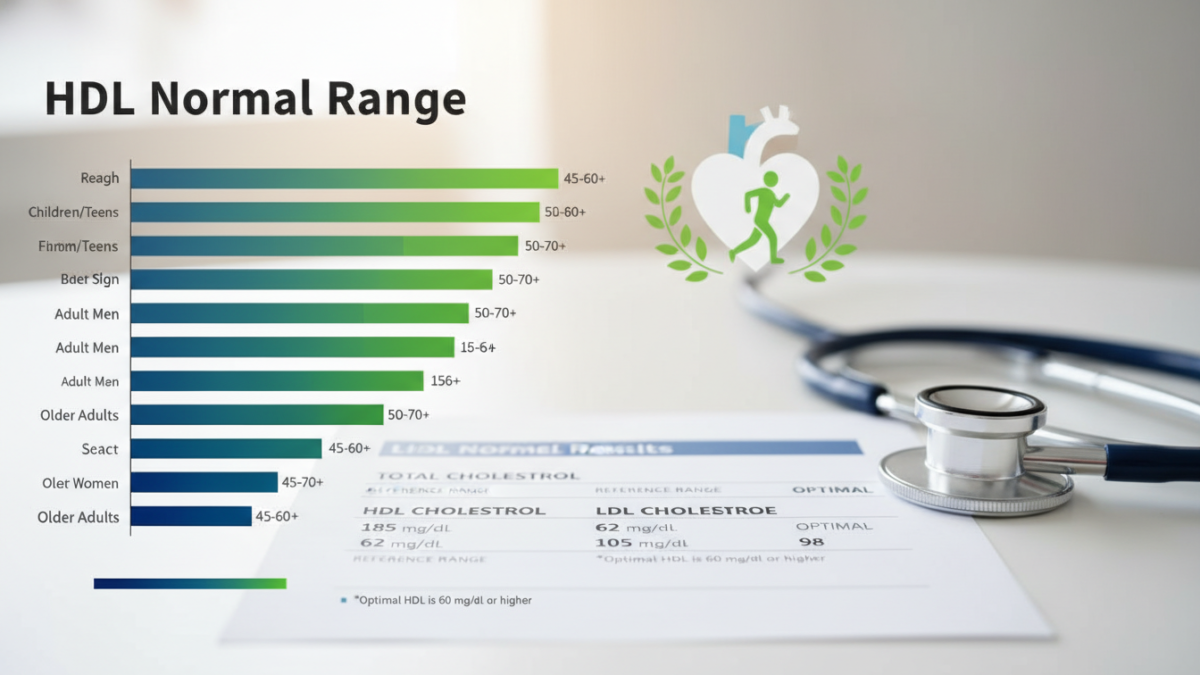
Knowing the HDL normal range is key to checking heart health. Men and women have different targets because of hormones and biology. The American Heart Association says 60 mg/dL or more is good for the heart.
Men: Healthy HDL Targets
For adult men, HDL levels should be between 40 and 70 mg/dL. Levels under 40 mg/dL are a big risk for heart disease. Men usually have lower HDL than women, thanks to testosterone.
Women: Healthy HDL Targets
Women’s HDL levels should be between 50 and 90 mg/dL. Estrogen helps women keep higher HDL. After menopause, estrogen drops, and HDL and LDL levels change.
According to the National Heart, Lung, and Blood Institute, an HDL level of 60 mg/dL or higher offers meaningful cardiovascular protection for both sexes.
Units of Measurement
In the U.S., HDL levels are measured in milligrams per deciliter (mg/dL). Other countries might use millimoles per liter (mmol/L). To convert mg/dL to mmol/L, divide by 38.67.
| Category | Men (mg/dL) | Women (mg/dL) | Risk Level |
|---|---|---|---|
| Low | Below 40 | Below 50 | Increased cardiovascular risk |
| Normal | 40–60 | 50–60 | Average risk |
| Optimal | 60–70 | 60–90 | Protective against heart disease |
Knowing these ranges helps understand what happens when HDL levels change. This is explored in the next sections.
Implications of High HDL Cholesterol Levels
High HDL levels are a good sign for your heart. HDL acts like a cleanup crew in your blood. It removes extra cholesterol from your arteries and takes it to your liver to get rid of it.
Potential Health Associations
Studies show that HDL levels above 60 mg/dL can protect your heart. Keeping your HDL levels healthy can lower your risk of heart disease. This includes reducing the risk of heart attacks and strokes.
Exercising regularly can also raise your HDL levels. Doing aerobic exercises 3–5 times a week can increase HDL by 5–10%. If you’re looking to manage your cholesterol, learning about cholesterol medication options is a good place to start.
High HDL levels offer several benefits:
- They remove LDL (“bad”) cholesterol from artery walls.
- They have anti-inflammatory effects on blood vessels.
- They reduce the oxidation of lipoproteins that damage arteries.
Conditions Linked to Elevated Levels
But, very high HDL levels, above 100 mg/dL, might not be as good. Research in the Journal of the American College of Cardiology (2022) found that very high levels might not protect your heart as much. They could be linked to genetic conditions or chronic alcohol use.
| HDL Level (mg/dL) | Classification | Cardiovascular Impact |
|---|---|---|
| Less than 40 (men) / 50 (women) | Low | Increased heart disease risk |
| 40–59 | Acceptable | Moderate protection |
| 60–99 | Optimal | Strong cardiovascular protection |
| 100+ | Very High | Protective benefit may diminish |
Knowing where your HDL levels fall helps you and your doctor understand your heart health. It guides decisions on treatment or lifestyle changes.
Implications of Low HDL Cholesterol Levels
When HDL levels drop, the body’s defense against artery plaque weakens. Knowing the HDL levels that are too low is key. It shows how much risk you have for heart disease. Low HDL means less cholesterol is removed from the blood and sent to the liver.
Health Risks Associated with Low HDL
The American Heart Association says HDL levels under 40 mg/dL in men and under 50 mg/dL in women are risky. Without enough HDL, LDL cholesterol builds up in artery walls. This causes blood vessels to harden and narrow.
“Low HDL cholesterol is one of the major risk factors for coronary heart disease, even when total cholesterol levels appear normal.” — National Heart, Lung, and Blood Institute
The National Institutes of Health says low HDL often comes with high triglycerides. This mix is dangerous and speeds up artery damage.
Conditions Linked to Decreased Levels
Many health issues and lifestyle choices can lower HDL:
- Type 2 diabetes — insulin resistance messes with lipid metabolism
- Cigarette smoking — it directly lowers HDL production
- Obesity — too much body fat changes how cholesterol moves
- Sedentary lifestyle — not moving enough reduces HDL
- Metabolic syndrome — a group of conditions that lower HDL together
| Risk Factor | Estimated HDL Reduction | Reversible? |
|---|---|---|
| Cigarette Smoking | 5–10 mg/dL | Yes, within weeks of quitting |
| Physical Inactivity | 5–8 mg/dL | Yes, with regular aerobic exercise |
| Obesity (BMI over 30) | 5–15 mg/dL | Yes, with sustained weight loss |
| Uncontrolled Type 2 Diabetes | 5–12 mg/dL | Partially, with blood sugar management |
Knowing about HDL levels helps doctors create better treatment plans. Changing things like smoking, exercise, and weight can improve HDL levels. This is discussed further in the next sections on related biomarkers and lifestyle changes.
Related Biomarkers in Cholesterol Testing
Knowing about HDL levels is key, but it’s just part of the cholesterol story. A standard lipid panel checks several biomarkers at once. Each one gives a different view of heart health. Doctors look at all of them to understand the whole picture.

Total Cholesterol
Total cholesterol shows the total amount of cholesterol in the blood. It includes HDL, LDL, and other types like VLDL. The National Heart, Lung, and Blood Institute says a good total cholesterol level is under 200 mg/dL.
Doctors use total cholesterol to figure out non-HDL cholesterol. This is total cholesterol minus HDL. It shows all the “bad” cholesterol types in one number.
LDL Cholesterol
LDL is called “bad” cholesterol because it builds up plaque in artery walls. This buildup can narrow blood vessels and increase the risk of heart attack and stroke. Most adults should aim for an LDL level of 100 mg/dL or less.
If LDL is high and HDL is not in the optimal range, the risk of heart disease goes up.
Triglycerides
Triglycerides are the most common fat in the body. They come from extra calories the body doesn’t use right away. Here’s how triglyceride levels are classified:
| Triglyceride Level (mg/dL) | Classification |
|---|---|
| Below 150 | Normal |
| 150–199 | Borderline High |
| 200–499 | High |
| 500 or above | Very High |
High triglycerides and low HDL often go together in metabolic syndrome. Looking at all lipid panel results together is the best way to understand a person’s heart health risk.
Factors Influencing HDL Cholesterol Levels
Many things affect HDL cholesterol levels. What we eat, how we exercise, and our genes all play a part. Knowing these factors can help us keep our HDL levels healthy and lower heart disease risk.
Dietary Influences
Our diet directly affects HDL levels. Foods high in saturated fat can change blood cholesterol levels. The American Heart Association suggests eating less than 6% of daily calories as saturated fat.
Switching to unsaturated fats like olive oil, nuts, and fatty fish can help. These foods support healthy HDL levels.
Lifestyle Factors
Being inactive is a heart disease risk. Regular aerobic exercise, at least 150 minutes a week, can boost HDL. It helps stay within the HDL normal range.
Body weight also affects HDL levels. Excess weight, mainly around the midsection, lowers HDL and raises LDL. Quitting smoking also raises HDL levels quickly.
- Engage in brisk walking, cycling, or swimming most days of the week
- Maintain a healthy body weight
- Avoid tobacco use in any form
- Limit alcohol intake to moderate amounts
Genetic Factors
Genes influence cholesterol production and processing. High cholesterol can run in families, known as familial hypercholesterolemia. Race and ethnicity also affect risk.
The CDC notes Asian Americans often have high LDL levels. Non-Hispanic White adults tend to have high total cholesterol. Personalized strategies, guided by a healthcare provider, may be needed to maintain healthy HDL levels.
Clinical Context Considerations for HDL Testing
Looking at HDL levels isn’t just about a number. Your age, sex, and health status matter too. Doctors use these factors to understand what your HDL levels really mean.
Age and Gender Differences
Cholesterol levels often go up with age. Even kids and teens can have unhealthy cholesterol levels. This is why early testing is important.
Men between 20 and 39 are more likely to have high total cholesterol than women of the same age. But, after menopause, women’s cholesterol levels can change. Lower estrogen levels can drop HDL and raise LDL, increasing heart disease risk.
Doctors recommend more frequent testing for women after 55 because of these changes.
The testing schedule depends on your age:
| Age Group | Recommended Testing Frequency |
|---|---|
| Adults aged 20–44 | Every 5 years |
| Men aged 45–65 | Every 1–2 years |
| Women aged 55–65 | Every 1–2 years |
| Adults over 65 | Annually |
Coexisting Health Conditions
Some health conditions can affect HDL test results. People with metabolic syndrome or type 2 diabetes often have high triglycerides and low HDL. This combo increases heart disease risk, the American Heart Association says.
Some medicines, like beta-blockers and steroids, can also lower HDL. Knowing about all your medications and health history helps doctors make better treatment plans.
Limitations of the HDL Cholesterol Test
Knowing your high-density lipoprotein range is important, but the HDL cholesterol test has its limits. A single test doesn’t show the whole picture of heart health. It’s key for both patients and doctors to consider several factors when looking at the results.

Variability in Measurements
HDL cholesterol results can change from one lab to another. This is because labs use different methods to test and calibrate. Things like age, gender, recent illness, and even the time of day can also affect the results.
Getting a blood test has some minor risks. These include:
- Slight stinging or pain at the needle site
- Bruising or soreness afterward
- Rare instances of infection or feeling lightheaded
Because of these natural changes, one test might not show a person’s true baseline. Testing again over time can give a clearer picture of where someone stands in the optimal HDL range.
Interpretation Challenges
Having an optimal HDL range doesn’t mean you’re completely safe from heart disease. HDL levels are just one part of a bigger picture. Other factors like total cholesterol, LDL cholesterol, triglycerides, blood pressure, family history, and lifestyle are also important.
“Cholesterol numbers should never be evaluated in isolation. The interplay between multiple biomarkers determines true cardiovascular risk.” — American Heart Association
New research from the National Institutes of Health shows that HDL functionality is key. It’s not just about how much HDL you have, but how well it works. Two people with the same HDL range could have very different risks based on how well their HDL works and other health conditions.
So, doctors should look at HDL results in a bigger picture. This is something we’ll dive into more in the next section on future research directions.
Future Directions in HDL Research
Scientists are now looking beyond just HDL numbers. They want to know how well HDL works. This new focus could change how doctors check for heart disease risk soon.
Emerging Studies on HDL Functionality
Studies from places like the National Heart, Lung, and Blood Institute show HDL quality is key. Even with the same HDL levels, people can have different heart health. Researchers are looking at HDL’s ability to remove cholesterol from arteries.
The 2018 ACC/AHA cholesterol guideline says “lower is better” for LDL-C. It shows that keeping LDL-C under 100 mg/dL can lower heart disease and stroke risks. For those who have had heart attacks, doctors aim for a 50% LDL-C drop, or 70 mg/dL or less. This shows HDL’s role in protecting the heart is important.
Potential for New Therapeutic Targets
Old drugs that raised HDL levels didn’t help heart health in trials. So, scientists are trying new approaches. They’re looking at ways to make HDL work better, not just increase its levels.
- CETP inhibitors that improve HDL particle quality
- ApoA-I infusion therapies that mimic HDL’s natural protective action
- Gene-based approaches targeting cholesterol transport pathways
These new ideas could change what we think of as normal HDL levels. It might not just be about a number anymore, but how well HDL protects the heart.
Conclusion
HDL cholesterol is key to keeping your heart healthy. Knowing how it works and checking your levels can help a lot.
How HDL Protects Your Cardiovascular System
This guide shows HDL’s importance. It helps remove bad cholesterol from your arteries. This action prevents plaque buildup and lowers heart disease risk.
When HDL levels are good, it works well with low LDL. Together, they help keep your heart safe.
“Heart disease remains the leading cause of death in the United States, claiming roughly 695,000 lives each year.” — Centers for Disease Control and Prevention
Keeping LDL low and HDL high is key to heart health. The American Heart Association agrees.
Why Regular Monitoring Matters
One HDL reading isn’t enough. The National Heart, Lung, and Blood Institute suggests regular lipid panels. Doctors look at HDL and other important factors:
- Age and gender
- Family history of heart disease
- Smoking status
- Blood pressure readings
- Presence of diabetes or metabolic syndrome
- Total cholesterol and triglyceride levels
Regular screenings give a full view of heart risk. Adults 20 and up should check their cholesterol every four to six years. Those with risk factors might need more frequent tests.
By following HDL guidelines and working with a doctor, you can keep your heart healthy. This way, you can protect your heart for many years.
References
This article uses trusted medical sources from across the United States. These sources provide reliable information on HDL levels and heart health.
Medical Sources and Literature on HDL Cholesterol
The National Heart, Lung, and Blood Institute, part of the National Institutes of Health, offers detailed guidelines on cholesterol management. These guidelines help doctors find the best HDL range for patients. They consider age, sex, and risk factors.
ClinicalTrials.gov lists studies on conditions like high cholesterol and other lipid disorders. This helps researchers and doctors stay updated.
The American Heart Association gives advice on cholesterol testing for adults. It suggests lifestyle changes and treatments to boost HDL levels. The StayWell Company LLC provides materials on HDL testing and results for patients and doctors.
It’s important to check these sources for the latest on HDL levels and ranges. A healthcare provider can give personalized advice based on the newest research.