A cholesterol test is very common in health checks. It shows how much cholesterol is in your blood and what carries it. This simple test is key to checking your heart health.
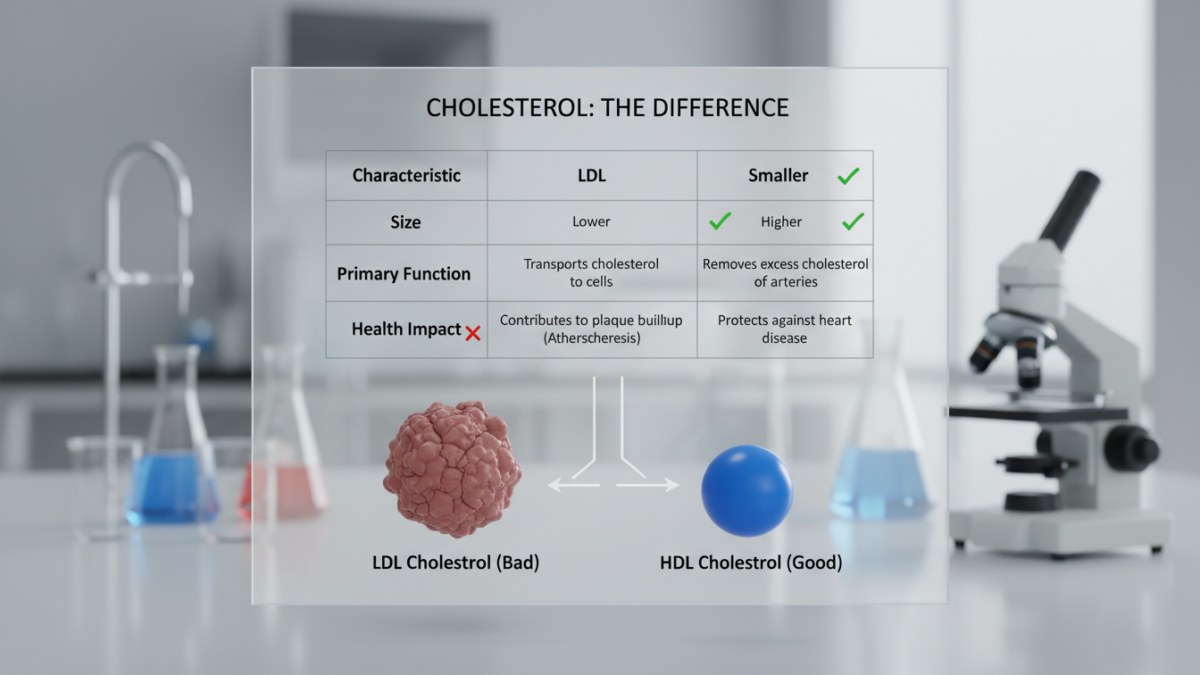
LDL and HDL cholesterol have different effects. LDL, or “bad” cholesterol, can clog arteries. This can lead to heart attacks and strokes.
On the other hand, HDL, or “good” cholesterol, helps clean arteries. It carries cholesterol back to the liver for removal. HDL is a small part of your total cholesterol.
Cholesterol is needed for cell growth and hormone production. It needs lipoproteins to move through the blood. High LDL levels might mean you need cholesterol medication to keep your heart safe.
Knowing about LDL and HDL helps you make better lifestyle choices. A healthy lipid profile is a strong defense against heart disease.
Key Takeaways
- Low density lipoprotein (LDL) deposits cholesterol on artery walls, earning its label as “bad” cholesterol.
- High density lipoprotein (HDL) removes excess cholesterol from arteries and sends it back to the liver for disposal.
- The LDL vs HDL difference directly influences a person’s risk for heart attack and stroke.
- Plaque buildup from high LDL narrows blood vessels and can lead to atherosclerosis.
- Only a small portion of total cholesterol is carried by HDL, making it important to track both numbers.
- A routine cholesterol blood test is one of the most reliable tools for evaluating cardiovascular risk.
What the Test Measures
A cholesterol test checks the amount of different fats in the blood. It’s not just one number. A complete lipid profile breaks down the results into specific parts. This gives doctors a clearer view of heart health.
Over one-third of Americans have high cholesterol levels. This makes the test very common in the United States.
Understanding LDL Cholesterol
LDL, or low-density lipoprotein, is the biggest part of cholesterol in the body. It carries cholesterol to the arteries. This can build up and narrow blood vessels, increasing the risk of heart disease and stroke.
The body makes about 75% of its cholesterol naturally. Diet makes up the remaining 25%. Foods high in saturated and trans fats can raise LDL levels over time.
Understanding HDL Cholesterol
HDL, or high-density lipoprotein, does the opposite. It absorbs excess cholesterol and takes it back to the liver. Higher HDL levels mean a lower risk for heart disease. That’s why HDL is called “good” cholesterol.
Importance of Lipid Profile
Dr. Parveen Garg from the USC Cardiac and Vascular Institute says it’s important to look at each part of the lipid profile. A full lipid profile includes LDL, HDL, and triglycerides. Each part gives unique insights into heart health.
| Lipid Profile Component | Primary Role | Impact on Heart Health |
|---|---|---|
| LDL Cholesterol | Delivers cholesterol to arteries | High levels increase risk |
| HDL Cholesterol | Removes cholesterol from blood | High levels decrease risk |
| Triglycerides | Stores unused calories as fat | High levels increase risk |
Understanding each part of the lipid profile helps patients and doctors create a plan. This plan protects long-term heart health and manages cholesterol levels effectively.
Why It Is Ordered
Doctors order cholesterol tests for certain reasons. They want to know about good and bad cholesterol levels. This helps them make treatment plans and spot problems early.
Risk Assessment for Cardiovascular Disease
High bad cholesterol and low good cholesterol increase heart attack and stroke risk. LDL cholesterol builds up in arteries, causing plaque. This narrows blood flow.
The American Heart Association says elevated triglycerides and bad cholesterol ratios make this risk even higher.
A lipid panel helps doctors check heart disease risk. It shows which cholesterol parts need work. This decides if lifestyle changes or medicine are needed.
Routine Health Screening
Cholesterol screening is key in preventive care in the U.S. How often depends on age and risk factors.
| Age Group | Recommended Frequency | Key Consideration |
|---|---|---|
| 18–39 years | Every 5 years | Baseline levels of good cholesterol and bad cholesterol established |
| 40–54 years | Every 1–2 years | Increased metabolic risk with age |
| 55–64 years | Every 1–2 years | Higher prevalence of lipid abnormalities |
| 65 years and older | Annually | Greatest cardiovascular risk window |
These guidelines are from the U.S. Preventive Services Task Force. People with diabetes, obesity, or heart disease history may need more frequent testing. Regular checks catch bad cholesterol increases and good cholesterol drops early.
Normal Reference Range
Understanding target cholesterol levels helps make sense of test results. The LDL vs HDL difference is clear when numbers are compared. Remember, what’s healthy varies by age, family history, and heart health.
LDL Cholesterol Levels (mg/dL)
LDL is called “bad” cholesterol because it builds up in artery walls. The American Heart Association says most adults should aim for an LDL of 100 mg/dL or less. Levels between 100 and 129 mg/dL are near optimal, but above 160 mg/dL is a concern.
Those with heart disease might need their LDL below 70 mg/dL. This requires medication and lifestyle changes.
HDL Cholesterol Levels (mg/dL)
HDL is like a cleanup crew, removing excess fat from the body. Men should aim for at least 40 mg/dL, and women for 50 mg/dL or higher. HDL levels of 60 mg/dL and above protect against heart disease.
The key is: lower is better for LDL, and higher is better for HDL.
| Marker | Optimal | Borderline | High Risk |
|---|---|---|---|
| LDL Cholesterol | Less than 100 mg/dL | 130–159 mg/dL | 160 mg/dL or above |
| HDL Cholesterol (Men) | 60 mg/dL or above | 40–59 mg/dL | Below 40 mg/dL |
| HDL Cholesterol (Women) | 60 mg/dL or above | 50–59 mg/dL | Below 50 mg/dL |
| Total Cholesterol | Less than 200 mg/dL | 200–239 mg/dL | 240 mg/dL or above |
| Triglycerides | Less than 150 mg/dL | 150–199 mg/dL | 200 mg/dL or above |
A doctor will look at these levels and personal risk factors to suggest treatment. This approach ensures each patient gets the right care for their heart health.
What High Levels May Indicate
High cholesterol levels can be a warning sign for serious health issues. When LDL levels get too high or HDL levels get too low, the body is at risk. It’s important to understand these changes to protect your heart health.
Implications of High LDL Levels
High LDL in the blood can start a dangerous process. LDL particles stick to artery walls, creating fatty streaks that turn into plaque. This narrows arteries and cuts off blood flow.
As plaque grows, the chance of heart attacks and strokes goes up. The American Heart Association says nearly half of American adults have heart disease. High LDL is a big risk factor that can be changed.
“Lowering LDL cholesterol is one of the most important things a person can do to reduce the chance of heart disease and stroke.” — American Heart Association
High LDL levels can lead to:
- Plaque rupture and blood clots
- Less oxygen to the heart muscle
- Higher risk of peripheral artery disease
Implications of Low HDL Levels
HDL is key for heart health because it helps remove excess cholesterol. If HDL levels drop below 40 mg/dL in men or 50 mg/dL in women, the body loses a vital defense.
Low HDL means less LDL is removed from the blood. Remember, high HDL does not make up for high LDL. Both numbers need to be in the normal range for good heart health.
What Low Levels May Indicate
Not all cholesterol readings are a cause for worry. Sometimes, the numbers on a lipid panel show strong heart health. When LDL is low and HDL is high, the body fights heart disease better.
Implications of Low LDL Levels
Low LDL cholesterol is good news for most people. It means less “bad” cholesterol in the blood. This slows down plaque buildup in arteries.
The American Heart Association says keeping LDL below 100 mg/dL lowers heart attack and stroke risks. People with diabetes, high blood pressure, or heart disease family history benefit most.
Implications of High HDL Levels
High HDL cholesterol acts as a defense. It picks up LDL from artery walls and takes it to the liver. The liver then breaks it down and removes it.
More good cholesterol means a more efficient cleanup process. Levels above 60 mg/dL protect against heart disease, as the National Institutes of Health note.
It’s key to know that HDL cannot reverse hardened plaque in arteries. Its role is to prevent, not fix. The best scenario is high HDL with controlled LDL for heart protection.
| Cholesterol Marker | Desirable Level (mg/dL) | Cardiovascular Effect |
|---|---|---|
| Low LDL | Below 100 | Reduced plaque buildup |
| High HDL | Above 60 | Improved cholesterol removal |
| Optimal Combination | LDL <100, HDL >60 | Strongest heart protection |
Knowing these markers helps doctors and patients make better treatment plans. It connects to the biomarkers discussed next.
Related Biomarkers
A complete lipid profile is more than just LDL and HDL numbers. It includes other important biomarkers that show more about heart health. These measurements help doctors understand a patient’s risk for heart disease and stroke.

Total Cholesterol Measurements
Total cholesterol measures all cholesterol in the blood. It combines LDL, HDL, and some triglycerides into one number. The American Heart Association says a total cholesterol under 200 mg/dL is good.
But, total cholesterol alone isn’t enough. A high total number can be due to high HDL, which is good. That’s why looking at each part of the lipid profile is key for accurate risk assessment.
Triglycerides and Their Significance
Triglycerides are the main fat in our bodies. They store extra calories as energy. If we eat more than we burn, our triglycerides go up.
High triglycerides with high LDL or low HDL increase heart attack and stroke risk. This is because they lead to fatty deposits in artery walls.
| Triglyceride Level (mg/dL) | Category | Heart Risk |
|---|---|---|
| Below 150 | Normal | Low |
| 150–199 | Borderline High | Moderate |
| 200–499 | High | Elevated |
| 500 and above | Very High | Severe |
Triglycerides are the third pillar of cholesterol testing. Along with LDL and HDL, they provide a full view of heart health. This is vital for making treatment plans and lifestyle changes that improve long-term health.
Factors That Affect Results
Your cholesterol levels don’t exist in a vacuum. Many factors, from what you eat to how well you sleep, can change your lipid profile. This is why test results can vary.
Diet Impact on Cholesterol Levels
What you eat directly affects your bad cholesterol. Foods high in saturated fats, trans fats, and processed foods raise LDL. Red meat, full-fat dairy, and fried foods are bad choices.
On the other hand, foods high in soluble fiber like oats, beans, and fruits can lower cholesterol.
“Dietary changes remain one of the most effective first-line strategies for managing elevated LDL cholesterol.” — American Heart Association
Lifestyle Factors Affecting Lipid Profiles
Age and gender also play a role. Cholesterol levels rise with age. Women often see a spike in bad cholesterol after menopause due to declining estrogen.
Genetics, race, and family history also matter. These factors can influence your cholesterol levels.
Chronic stress and poor sleep can also affect cholesterol levels. Stress hormones like cortisol encourage fat storage and can lead to unhealthy eating. Lack of sleep increases inflammation, raising cardiovascular risk.
| Factor | Effect on LDL (Bad Cholesterol) | Effect on HDL (Good Cholesterol) |
|---|---|---|
| High saturated fat diet | Increases | Minimal change |
| Regular exercise | Decreases | Increases |
| Smoking | Increases | Decreases |
| Chronic stress | Increases | Decreases |
| Obesity | Increases | Decreases |
| Quitting smoking | Decreases over time | Increases within weeks |
Diabetes, obesity, and high blood pressure can worsen the effects of bad cholesterol on heart health. Quitting smoking is one of the fastest ways to improve HDL, often showing results within just a few weeks.
Clinical Context Considerations
Cholesterol numbers don’t tell the whole story. Doctors look at a patient’s complete health picture before deciding on treatment. The LDL vs HDL difference is important, but it’s even more meaningful when seen with other health details like age, gender, and existing conditions.
Correlation with Other Risk Factors
Abnormal cholesterol becomes more dangerous when combined with other risk factors. For example, someone with high LDL and type 2 diabetes is at a higher risk than someone with high LDL alone. The American Heart Association lists several conditions that increase risk when combined with poor lipid numbers:
- High blood pressure (hypertension)
- Type 2 diabetes or insulin resistance
- Obesity, with a focus on excess abdominal fat
- Active smoking or tobacco use
- A sedentary lifestyle with little physical activity
Each of these factors adds to the overall risk. For heart health, managing cholesterol means tackling all these risks, not just one number on a lab report.
“Cardiovascular risk assessment must account for the totality of a patient’s risk profile, not isolated biomarkers.” — 2019 ACC/AHA Guideline on Primary Prevention of Cardiovascular Disease
Importance of Family History
Genetics play a big role in cholesterol production and processing. A family history of early heart disease, like in a parent or sibling before age 55 for men or 65 for women, increases risk a lot.
Conditions like familial hypercholesterolemia can cause very high LDL levels, even with a good diet and exercise. Women should know that hormonal changes after menopause can make their lipid profiles worse, making the LDL vs HDL difference less favorable.
A personalized approach to heart health takes all these factors into account. Treatment plans based on family history, current lifestyle, and other health conditions lead to the best results for each patient.
Limitations of the Test
No single cholesterol test tells the full story of a person’s heart health. Unlike a fever that clearly signals illness, cholesterol levels lack a universal threshold that applies to every individual. A lipid profile offers valuable data, but it comes with important limitations that both patients and clinicians should understand.
Variability in Results
Cholesterol levels can change from one blood draw to the next. Recent meals, stress, illness, and even the time of day can affect results. The Journal of Clinical Lipidology notes that LDL cholesterol can vary up to 10% between tests weeks apart.
This natural variability means a single lipid profile snapshot may not reflect a person’s true baseline. Doctors often recommend repeat testing before making treatment decisions. Seasonal changes can also play a role — research shows cholesterol levels tend to be higher in winter months.
Interpretation of Results
Reading cholesterol levels in isolation creates an incomplete picture. A person with high HDL does not automatically cancel out the risks tied to elevated LDL. HDL helps remove circulating bad cholesterol, but it cannot reverse plaques that have already built up inside artery walls.
Accurate interpretation requires looking at the full context:
- Age, sex, and ethnicity influence what counts as “normal”
- Existing conditions like diabetes or hypertension change risk thresholds
- Family history of heart disease may demand stricter targets
- Medications such as statins or steroids can alter results
A lipid profile is one piece of a larger puzzle — not a standalone diagnosis.
Focusing on total numbers alone, without examining each component of the lipid profile, can lead to misleading conclusions. Clinicians weigh cholesterol levels alongside other biomarkers and personal risk factors covered in earlier sections to form a complete assessment.
References
This article uses trusted medical sources. It talks about the main differences between low density lipoprotein and high density lipoprotein. For more on managing cholesterol and heart health, readers can check out these resources.
Medical Journals and Guidelines
The National Heart, Lung, and Blood Institute (NHLBI) has guidelines on high blood cholesterol. The USDA Dietary Guidelines for Americans 2020–2025 give advice on fats and cholesterol. Dr. Parveen Garg of USC Cardiac and Vascular Institute at Keck Medicine of USC shares insights on low density lipoprotein and heart risk.
MedlinePlus, a National Library of Medicine service, is a great place for cholesterol health info.
Authoritative Health Organizations
The American Heart Association, updated on February 19, 2024, is a top source for cholesterol advice. It explains how high density lipoprotein protects us. The Centers for Disease Control and Prevention (CDC), updated on May 14, 2024, offers tips on preventing heart disease and stroke related to cholesterol.
These groups help both patients and doctors make smart choices about testing and treatment.