The lipid panel test is a key test in health care. It checks fats in your blood. Doctors use it to see if you might get heart disease or stroke.
This test looks at four important markers: total cholesterol, LDL, HDL, and triglycerides. It helps doctors and patients make better choices about diet and exercise.
Our liver makes cholesterol and removes extra. Foods like red meat and full-fat dairy can increase cholesterol. High levels can cause arteries to narrow.
How you interpret lipid panel results depends on your age and health history. The American Heart Association suggests testing every four to six years for most adults. Those with high cholesterol or heart issues might need more frequent tests.
Key Takeaways
- A lipid panel measures total cholesterol, LDL, HDL, and triglycerides in one blood test.
- Results are reported in milligrams per deciliter (mg/dL) and help gauge cardiovascular disease risk.
- The liver produces cholesterol naturally, but dietary sources from animal products can push levels higher.
- Lipid panel interpretation requires context — age, family history, and existing conditions all matter.
- Low-risk adults should have cholesterol levels checked every four to six years starting at age 20.
- Understanding lipid test results empowers patients to take early action against heart disease and stroke.
What the Test Measures
A lipid panel breaks down fats in your blood into specific categories. Each category helps patients and doctors understand heart health better. The test reports four key markers that show your risk for heart disease.
Total Cholesterol
Total cholesterol is a mix of HDL, LDL, and 20% of triglycerides. The American Heart Association says an optimal level is around 150 mg/dL. This number gives a quick look, but it’s not the whole story.
Low-Density Lipoprotein (LDL)
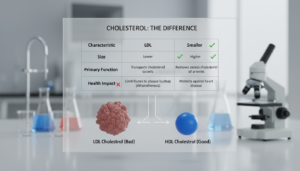
LDL is called the “bad” cholesterol. It builds up fat in artery walls, leading to plaque and narrowed blood vessels. High LDL is a big risk for heart disease.
High-Density Lipoprotein (HDL)
HDL is the “good” cholesterol. It carries excess fat back to the liver. Higher HDL levels mean lower heart attack and stroke risks. It’s a protective part of your lipid profile.
Triglycerides
Triglycerides store calories and give energy to cells. Their levels change with what you eat and drink. A triglycerides analysis shows how your body handles fats and sugars. VLDL, which carries fats, is not directly measured but can be estimated from triglyceride levels.
| Component | Primary Role | Impact on Heart Health |
|---|---|---|
| Total Cholesterol | Overall fat measurement | General risk indicator |
| LDL | Delivers cholesterol to arteries | Increases plaque buildup |
| HDL | Returns cholesterol to the liver | Reduces cardiovascular risk |
| Triglycerides | Stores and supplies energy | Elevates risk when high |
Understanding each marker is key to knowing why doctors order this test. This is explored further in the next section on cardiovascular risk assessment.
Why the Test is Ordered
Doctors order a lipid panel for several important reasons. It helps paint a complete picture of a patient’s health. This blood test is vital for both healthy adults and those with ongoing health issues. It guides doctors in making key treatment decisions.
Assessing Cardiovascular Risk
One main reason for lipid testing is to assess cardiovascular risk. Doctors look at lipid levels, age, smoking, diabetes, and blood pressure. This helps predict the risk of heart attack or stroke.
Plaque buildup in arteries, or atherosclerosis, can cause serious problems. The American Heart Association suggests screening every four to six years for adults over 20 with average risk.
Monitoring Treatment Efficacy
For those on cholesterol-lowering drugs, lipid panels show if the treatment is working. Doctors compare current levels to baseline values. If levels are not improving, treatment might need to change.
Testing frequency often increases to every three to twelve months during active treatment.
Evaluating Metabolic Disorders
A lipid panel is key in identifying metabolic disorders. High triglycerides, low HDL, and high blood sugar may indicate metabolic syndrome. This condition significantly increases heart disease risk.
By analyzing lipid panel data, doctors can spot these patterns early.
| Reason for Ordering | Key Focus | Typical Testing Frequency |
|---|---|---|
| Cardiovascular risk assessment | Heart attack and stroke prevention | Every 4–6 years (average risk) |
| Treatment monitoring | Medication effectiveness | Every 3–12 months |
| Metabolic disorder evaluation | Metabolic syndrome detection | Annually or as clinically indicated |
Normal Reference Range
It’s key to know the lipid panel reference ranges to understand test results. These numbers show if a patient’s cholesterol and triglyceride levels are healthy. The American Heart Association and the National Institutes of Health set guidelines for adults 20 and older.
Total Cholesterol Levels (mg/dL)
For adults, total cholesterol should be under 200 mg/dL to be considered normal. Levels between 200 and 239 mg/dL are borderline high. Anything over 240 mg/dL is high. For those 19 or younger, the goal is less than 170 mg/dL.
LDL Cholesterol Levels (mg/dL)
LDL, or “bad” cholesterol, has specific guidelines:
| Category | LDL Level (mg/dL) |
|---|---|
| Optimal | Less than 100 |
| Near Optimal | 100–129 |
| Borderline High | 130–159 |
| High | 160–189 |
| Very High | 190 and above |
For kids and teens, LDL under 100 mg/dL is good.
HDL Cholesterol Levels (mg/dL)
HDL, or “good” cholesterol, helps remove LDL. The ranges vary by sex:
- Men: 40 mg/dL or higher
- Women: 50 mg/dL or higher
- Both: 60 mg/dL and above is protective against heart disease
Triglyceride Levels (mg/dL)
Triglycerides should be under 150 mg/dL for normal levels. Levels between 150 and 199 mg/dL are borderline high. High levels are 200 to 499 mg/dL, and very high is 500 mg/dL or more. High triglycerides can signal risks beyond heart disease.
What High Levels May Indicate
High lipid levels in a lipid panel analysis can signal health concerns. These concerns range from heart disease risk to metabolic issues. Knowing what these numbers mean is key to making effective treatment plans.
Increased Cardiovascular Risk
High cholesterol starts with LDL cholesterol. LDL levels above 190 mg/dL may indicate familial hypercholesterolemia. This genetic condition increases the risk of heart attacks and strokes.
The American College of Cardiology has clear LDL goals. These goals depend on your risk level:
| Patient Category | Recommended LDL Goal |
|---|---|
| No heart disease | Below 100 mg/dL |
| Existing heart disease | Below 70 mg/dL |
| Heart disease plus extra risk factors | Below 55 mg/dL |
Lipoprotein(a) levels above 125 nmol/L (or 50 mg/dL) also increase cardiovascular risk. This is true regardless of other cholesterol values.
Possible Metabolic Syndrome
Elevated lipid levels often signal metabolic syndrome or diabetes. High triglycerides, LDL, and low HDL are warning signs. Triglycerides over 500 mg/dL can lead to pancreatitis, a serious inflammation of the pancreas.
Other Associated Conditions
Abnormal lipid panel results can indicate more than just heart disease. These include:
- Hypothyroidism (underactive thyroid)
- Chronic kidney disease
- Liver disorders
- Certain medications, such as corticosteroids or diuretics
Interpreting high cholesterol requires looking at the whole picture. Doctors consider lifestyle, family history, and other biomarkers when making treatment plans.
What Low Levels May Indicate
Many people worry about high cholesterol. But it’s also key to understand the importance of low cholesterol. Low cholesterol levels can signal health issues that need attention. It’s important to look at numbers below the normal range, not just above it.
Potential Nutritional Deficiencies
Very low total cholesterol might mean malabsorption or malnutrition. Our bodies need cholesterol for hormones, vitamin D, and bile acids. If we can’t absorb fats well, like with celiac disease, cholesterol levels can drop.
A cholesterol deficiency due to poor nutrition needs quick dietary checks.
Genetic Disorders
Some inherited conditions affect how we process lipids. Hypobetalipoproteinemia and abetalipoproteinemia lead to low cholesterol levels. These rare conditions can cause vitamin deficiencies and brain problems if not treated.
| Genetic Condition | Effect on Cholesterol | Key Complication |
|---|---|---|
| Hypobetalipoproteinemia | Very low LDL | Fatty liver disease |
| Abetalipoproteinemia | Near-absent LDL | Neurological damage |
| Tangier Disease | Extremely low HDL | Peripheral neuropathy |
Other Health Conditions
Low HDL levels increase heart disease risk. Diabetes, smoking, lack of exercise, and being overweight all lower HDL. Men usually have lower HDL than women until women reach menopause, around age 55.
Liver problems are another concern. The liver is key in making and recycling cholesterol. Hepatic dysfunction can lead to low readings. Hyperthyroidism and chronic infections can also cause low cholesterol. It’s important to consider these when looking at lipid test results.
Related Biomarkers
A standard lipid panel is a good start. But, some lipid biomarkers give a deeper look at heart disease risk. Advanced lipid analysis can spot dangers that simple tests might miss, helping those with complex health issues.

Apolipoprotein A1
Apolipoprotein A1 (ApoA1) is key in HDL cholesterol. It helps remove extra cholesterol from arteries. Low ApoA1 levels can mean a higher heart disease risk, even with normal HDL.
Apolipoprotein B
Apolipoprotein B (ApoB) counts all harmful lipoprotein particles in the blood. Each LDL particle has one ApoB molecule. This makes ApoB a direct measure of atherogenic particle count. Testing for ApoB is useful when LDL cholesterol doesn’t show the full risk — a problem in about 20% of people.
This issue is common in those who are overweight, have diabetes, or have metabolic syndrome. For those with familial hypercholesterolemia or LDL over 190 mg/dL with normal triglycerides, special tests show all LDL particles contribute to plaque buildup, regardless of size.
Lipoprotein(a)
Lipoprotein(a), or Lp(a), is a genetic risk factor for heart disease. It causes artery blockages, inflammation, and blood clots. High Lp(a) and LDL together increase heart disease risk, even with healthy HDL levels.
According to the American Heart Association, Lp(a) levels stay mostly the same throughout life. So, one test is usually enough for checking.
There are good reasons to ask for these lipid biomarkers through lipoprotein testing:
- Family history of early heart disease
- Unexplained heart problems despite normal LDL
- Suspected mismatch between LDL cholesterol and actual particle count
- Monitoring risk in patients with diabetes or obesity
| Biomarker | What It Measures | Optimal Range | Key Clinical Use |
|---|---|---|---|
| ApoA1 | Main HDL protein | 120–180 mg/dL | Assessing protective cholesterol function |
| ApoB | Atherogenic particle count | Below 90 mg/dL | Detecting LDL discordance |
| Lp(a) | Genetically driven risk factor | Below 30 mg/dL | Identifying inherited cardiovascular risk |
Understanding these markers through advanced lipid analysis helps doctors create better prevention plans. This is key when looking at the external factors discussed next.
Factors That Affect Results
A lipid panel doesn’t happen in isolation. Many things can change cholesterol levels, sometimes a lot. Knowing these factors helps us understand lab results better. Here are the main things to know about lipid panels.
Diet and Nutrition
What you eat greatly affects your cholesterol levels. Foods high in saturated and trans fats, like fried foods and red meat, can increase LDL. But, eating more fiber and healthy fats can lower LDL by 10–15% on average.
Triglycerides are affected by recent meals. Labs usually ask for a 9- to 12-hour fast before testing. Even a single drink can raise triglycerides in some people.
Physical Activity
Exercise is a big factor in improving lipid profiles. It lowers LDL, reduces triglycerides, and increases HDL. The American Heart Association suggests at least 150 minutes of moderate exercise weekly for healthy lipids.
Medications and Health Conditions
Some health issues can significantly affect cholesterol levels. These include:
- Underactive thyroid (hypothyroidism)
- Chronic kidney disease
- Pregnancy, specially in the third trimester
- Inflammatory conditions like rheumatoid arthritis
Stress also plays a role. It increases hormones that lead to more cholesterol. Some medicines, like beta-blockers and corticosteroids, can also change lipid levels.
| Factor | Primary Lipid Affected | Direction of Change |
|---|---|---|
| Saturated/trans fat intake | LDL | Increase |
| Regular aerobic exercise | HDL / Triglycerides | HDL rises / Triglycerides drop |
| Alcohol consumption | Triglycerides | Increase |
| Hypothyroidism | Total Cholesterol / LDL | Increase |
| Chronic stress | Total Cholesterol | Increase |
Clinical Context Considerations
Lipid panel numbers don’t tell the whole story. It’s important to look at each patient’s health profile. Doctors consider many factors before deciding on treatment based on test results.
Individual Risk Factors
Assessing heart disease risk goes beyond just looking at cholesterol numbers. Doctors check for smoking, diabetes, high blood pressure, obesity, and insulin resistance. They also consider chronic inflammation and heart disease risk.
The 2018 ACC/AHA Cholesterol Guidelines say “lower is better” for LDL-C. This is true, even more so when there are many risk factors.
Family History
A family history of heart disease is very important. Heart disease early in life is a big concern. Familial hypercholesterolemia, a genetic condition, needs close monitoring and early action.
Children with a family history of high cholesterol or heart disease may need tests as early as age 2. Most kids should get tested between ages 9 and 11.
Age and Gender Influences
Age and gender affect cholesterol levels. Women usually have lower LDL until menopause, around age 55. Men have lower HDL levels at all ages.
| Age Group | Recommended Testing Frequency | Key Gender Consideration |
|---|---|---|
| 20–44 years | Every 5 years | Men often show higher LDL earlier |
| Men 45–65 / Women 55–65 | Every 1–2 years | Post-menopausal women see rising LDL |
| Over 65 years | Annually | Both sexes face elevated cardiovascular risk |
Considering age, gender, and personal history is key. It helps doctors find the best ways to prevent and treat heart disease.
Limitations of the Test
No lab test tells the full story on its own. It’s key for patients and doctors to understand lipid panel limitations. Several factors can affect test results, leading to incomplete or misleading conclusions.
Misinterpretation of Results
A normal total cholesterol reading can hide high LDL levels. This is a common challenge in clinical practice. To accurately assess cardiovascular risk, it’s important to look at LDL, HDL, and triglycerides individually.
“A single number never captures the complexity of a patient’s metabolic health. Context is everything.”
Just looking at one number without considering other risk factors can lead to missed diagnoses or unnecessary treatments.
Variability in Testing Methods
LDL cholesterol can be reported in two ways: as a calculated estimate or a direct measurement. Each method has its own limitations:
| Method | How It Works | Key Limitation |
|---|---|---|
| Calculated LDL (Friedewald Equation) | Estimated from total cholesterol, HDL, and triglycerides | Inaccurate when triglycerides exceed 400 mg/dL |
| Direct LDL Measurement | Measured independently in the lab | Higher cost and not always available |
At-home testing kits provide quick results but should be confirmed by a certified lab when total cholesterol is over 200 mg/dL.
Timing of Sample Collection
Triglyceride levels change throughout the day. Eating, exercise, and stress can significantly affect results. Fasting for 9 to 12 hours is critical for accurate readings.
- Non-fasting samples may inflate triglyceride readings
- Morning draws tend to produce the most consistent results
- Recent illness or medication changes can skew lipid values
Understanding these limitations helps patients and doctors interpret results better. This is important for making informed health decisions.
Conclusion
A lipid panel is key in checking heart health. Heart disease is the top killer in the U.S. So, checking cholesterol often is vital. Each part of the panel — total cholesterol, LDL, HDL, and triglycerides — gives a clue to health.
The American Heart Association says it’s important to keep LDL low and HDL high. The 2018 guidelines say “lower is better” for LDL. Doctors look at age, genetics, diet, exercise, and smoking to set targets for each patient.
Importance of Comprehensive Assessments
Doing a full lipid analysis is best when it’s part of a bigger check-up. Lipid panels are among the tests in guides to metabolic panels. These include CMP, BMP, liver function, iron studies, and glucose testing. Seeing lipid results with these tests helps doctors understand a patient’s health better.
Testing often helps catch problems early and adjust treatments. How often someone needs a test depends on their risk factors and heart health. Taking a holistic approach to risk helps patients and doctors make better choices for heart health.