A cholesterol blood test is very common in healthcare. It’s key for checking heart health. This test looks at cholesterol and triglycerides in the blood. It helps doctors see if you’re at risk for heart disease and stroke.
Cholesterol is a fatty substance in every cell. It’s needed for hormones, vitamin D, and digestion. The liver makes enough and removes extra.
For a cholesterol test, a healthcare worker takes a small blood sample. This is done after fasting for 9 to 12 hours. Now, you can also test at home with kits from LetsGetChecked and Everlywell. The results are in milligrams per deciliter (mg/dL).
A cholesterol test shows several important numbers. Each number tells us about blood fat levels. A lipid panel test looks at total cholesterol, LDL, HDL, and triglycerides. These numbers are important for planning your health.
Key Takeaways
- A cholesterol blood test, or lipid panel, measures cholesterol and triglyceride levels in the blood.
- The test requires fasting for 9 to 12 hours before blood is drawn.
- Cholesterol screening helps assess a person’s risk for heart disease and stroke.
- Results are measured in milligrams per deciliter (mg/dL) and include LDL, HDL, total cholesterol, and triglycerides.
- The liver produces all the cholesterol the body needs and removes excess amounts.
- At-home testing kits offer a convenient alternative to lab visits for basic lipid panel testing.
What the Test Measures
A cholesterol blood test, also known as a lipid panel, breaks down several key fats in the blood. It shows what each part means for heart health. This test gives a snapshot of cholesterol levels and fat markers.
Total Cholesterol
This number shows the total amount of cholesterol in the blood. It includes HDL and LDL levels, plus about 20% of triglycerides. A single total cholesterol reading gives a broad picture, but doctors need the full breakdown to assess risk accurately.
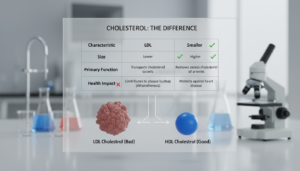
Low-Density Lipoprotein (LDL)
LDL is known as “bad” cholesterol. It builds up along artery walls and forms plaque. This condition, called atherosclerosis, narrows blood vessels and raises the risk of heart attack or stroke. Keeping LDL in check is a top goal in managing cholesterol levels.
High-Density Lipoprotein (HDL)
HDL is called “good” cholesterol because it carries LDL away from the arteries. The liver then removes it from the body. Higher HDL and LDL levels in a healthy range protect the cardiovascular system.
Triglycerides
Triglycerides are the most common type of fat in the blood. The body converts extra calories, sugar, and alcohol into triglycerides and stores them in fat cells. Elevated triglycerides, with high LDL or low HDL, can increase cardiovascular risk.
Labs may estimate VLDL (very low-density lipoprotein) using triglyceride data. Non-HDL cholesterol, which includes LDL and VLDL, offers another useful metric. Together, these markers give clinicians a detailed view that helps guide the next steps in care, as explored in the sections below on normal ranges and risk factors.
Why It Is Ordered
Doctors order a cholesterol blood test for several important reasons. It helps both patients and doctors make informed decisions about heart health. This test is a key part of preventive care for all ages.
Routine Health Check-Ups
A lipid panel is a standard part of preventive medicine. The American Heart Association recommends that adults aged 20 or older get their cholesterol checked every four to six years if their risk stays low. Children should first be tested between ages 9 and 11, with retesting every five years. Kids with a family history of high cholesterol may begin screening as early as age 2.
One of the most common cholesterol blood test FAQs is how often someone needs to be tested. The answer depends on age and risk level:
| Age Group | Recommended Frequency |
|---|---|
| Children (ages 9–11) | Once, then every 5 years |
| Adults (ages 20–44) | Every 4–6 years |
| Men (ages 45–65) | Every 1–2 years |
| Women (ages 55–65) | Every 1–2 years |
| Adults over 65 | Annually |
Risk Assessment for Cardiovascular Disease
Cholesterol test results give doctors essential data to evaluate a person’s risk for heart attacks, strokes, and peripheral artery disease. When combined with blood pressure readings, family history, and lifestyle factors, a lipid panel helps create a complete cardiovascular risk profile. Early detection through screening can lead to life-saving interventions.
Monitoring Cholesterol Levels over Time
For individuals already diagnosed with high cholesterol or those taking statin medications, regular testing tracks progress. Reviewing cholesterol blood test FAQs reveals that high-risk patients often need testing more frequently than standard guidelines suggest — sometimes every three to six months. Tracking trends over time allows providers to adjust treatment plans and confirm that dietary or medication changes are working as intended.
Normal Reference Range
Knowing what’s “normal” in cholesterol tests is key. Each part of a lipid panel has its own range. These ranges help doctors check heart health and decide if treatment is needed. Remember, fasting for 9 to 12 hours before the test is important, as it affects triglyceride accuracy.
Total Cholesterol Levels (mg/dL)
The best total cholesterol level is around 150 mg/dL. Levels under 200 mg/dL are good. Between 200 and 239 mg/dL is borderline-high, and over 240 mg/dL is high.
LDL Cholesterol Levels (mg/dL)
The 2018 American Heart Association/American College of Cardiology guideline says “lower is better” for LDL-C. Keeping LDL at or below 100 mg/dL lowers heart disease and stroke risk. Those with heart attacks or strokes might aim for LDL of 70 mg/dL or lower with medication. LDL results can be calculated or direct from the blood.
| LDL Range (mg/dL) | Classification |
|---|---|
| Less than 100 | Optimal |
| 100–129 | Near Optimal |
| 130–159 | Borderline High |
| 160–189 | High |
| 190 and above | Very High |
HDL Cholesterol Levels (mg/dL)
HDL, or “good” cholesterol, helps remove LDL. For men, 40 mg/dL or higher is good; for women, it’s 50 mg/dL. HDL of 60 mg/dL or above is protective against heart disease. HDL levels vary by gender and age.
Triglyceride Levels (mg/dL)
Triglyceride levels change with age. For adults, under 150 mg/dL is normal. 150 to 199 mg/dL is borderline high, 200 to 499 mg/dL is high, and 500 mg/dL or above is very high. Fasting before the test is key for accurate triglyceride results. Looking at all four markers gives doctors a full picture of lipid health.
What High Levels May Indicate
When cholesterol levels go up, it’s a warning sign. Knowing your cholesterol numbers is important. High levels can mean serious health problems that need quick medical attention.

Increased Cardiovascular Risk
High LDL cholesterol can cause plaque to build up in arteries. This can narrow blood vessels and limit blood flow. Such issues can lead to heart attacks, strokes, and peripheral artery disease.
- Heart attack — when plaque blocks blood flow to the heart
- Stroke — when blockage cuts off blood supply to the brain
- Peripheral artery disease — when circulation to the arms or legs becomes restricted
The American Heart Association says nearly 94 million U.S. adults have total cholesterol levels over 200 mg/dL.
Conditions Associated with High Cholesterol
High cholesterol often comes with other health issues. People with diabetes or metabolic syndrome often have high triglycerides and low HDL. Several factors can raise these numbers.
| Category | Contributing Factors |
|---|---|
| Lifestyle | Physical inactivity, excessive alcohol, high sugar intake, processed foods, saturated fat consumption |
| Medical Conditions | Hypothyroidism, chronic kidney disease, insulin resistance, obesity |
| Inflammatory Diseases | Rheumatoid arthritis, lupus |
| Physiological | Third trimester of pregnancy |
Hyperlipidemia
Hyperlipidemia means having too much fat in the blood. It includes high LDL and triglycerides. This condition often runs in families. Doctors use this knowledge to create treatment plans that lower heart risk.
What Low Levels May Indicate
Most people focus on high numbers when reviewing cholesterol test results. But low cholesterol levels are just as important. If a test shows very low readings, it could mean there’s a health issue that needs to be checked.
Cholesterol is key for cell membranes, hormones, and brain function. If it’s too low, it can cause problems. Genetics, lifestyle, and health conditions can all affect cholesterol levels.
Potential Nutritional Deficiencies
Low cholesterol levels might mean you’re not getting enough nutrients. The body needs fats and nutrients to keep cholesterol balanced. Conditions like celiac disease or very low-fat diets can cause low cholesterol.
Being underweight or having an eating disorder can also lower total cholesterol. A lack of vitamins A, D, E, and K often goes with these low numbers.
Conditions Related to Low Cholesterol Levels
Some health issues are linked to low cholesterol. These include:
- Hyperthyroidism — an overactive thyroid speeds up cholesterol metabolism
- Liver disease — the liver produces most of the body’s cholesterol
- Chronic infections or sepsis
- Some forms of cancer, like blood cancers
- Adrenal insufficiency
A study in the Journal of the American College of Cardiology found low LDL levels might raise the risk of hemorrhagic stroke. Gender also plays a role, as women usually have lower LDL levels than men until they’re around 55 or go through menopause.
One cholesterol test doesn’t tell the whole story. Doctors look at other biomarkers too to understand your health fully.
Related Biomarkers
A standard lipid panel test gives the main cholesterol values. But, some patients need more insight into their heart health. Doctors might order special biomarker tests if the cholesterol results are unclear or if the patient’s health is complex. These markers give a clearer view of heart disease risk.

Lipoprotein(a)
Lipoprotein(a), or Lp(a), is a genetic form of LDL cholesterol. High Lp(a) levels raise the risk of heart attack and stroke, even with normal cholesterol. The American Heart Association says about 20% of Americans have high Lp(a) levels.
Genetics mostly decide Lp(a) levels, so it’s usually tested only once in a lifetime.
Apolipoproteins
Apolipoproteins are proteins that carry fats in the blood. Two important types are:
- Apolipoprotein B (ApoB) — found on LDL particles; higher levels mean higher heart disease risk
- Apolipoprotein A-1 (ApoA1) — found on HDL particles; higher levels are good for the heart
Many doctors think ApoB is a better predictor of heart events than LDL alone. It’s very useful when cholesterol results are close to the line.
High-Sensitivity C-Reactive Protein (hs-CRP)
hs-CRP measures low-grade inflammation in the body. Chronic inflammation is key in atherosclerosis. A level above 3.0 mg/L means higher heart risk, studies in The New England Journal of Medicine show.
Adding inflammation markers to cholesterol tests gives doctors a full picture of heart risk.
These biomarkers add value to routine cholesterol tests. They help doctors make better treatment plans, even when standard tests don’t show everything.
Factors That Affect Results
When looking at cholesterol test results, many things can change the numbers. Lifestyle and body changes can make a big difference. This is why it’s important to understand why your results might change.
Diet and Nutrition
What you eat greatly affects your cholesterol levels. Foods high in saturated fats and trans fats can raise the bad cholesterol. Eating fish, nuts, and whole grains can help lower it.
Being overweight can also affect your cholesterol. Losing weight can improve your numbers.
Physical Activity Levels
Exercise is key to better cholesterol levels. The American Heart Association suggests 30 minutes of activity daily. Even simple activities like brisk walking can help.
Stress can also impact your cholesterol. It can raise the hormones that increase cholesterol production.
Age and Gender
Cholesterol levels increase with age. Men generally have higher cholesterol than women. Women see a big increase after menopause.
Some medications can also raise triglycerides. This is important to consider when looking at your results.
| Factor | Effect on LDL | Effect on HDL | Effect on Triglycerides |
|---|---|---|---|
| High saturated fat diet | Increases | Minimal change | Increases |
| Regular exercise (30 min/day) | Decreases | Increases | Decreases |
| Aging (over 50) | Increases | May decrease | Increases |
| Menopause in women | Increases | May decrease | Increases |
| Chronic stress | Increases | Minimal change | Increases |
Understanding these factors is important when looking at your cholesterol test results. It helps you talk to your doctor about what to do next.
Clinical Context Considerations
A single cholesterol number doesn’t tell the whole story. Doctors look at many personal and medical factors before deciding on treatment. It’s key to understand cholesterol test fasting needs and how HDL and LDL levels fit into a bigger health picture for accurate risk assessment.
Family History of Cholesterol Issues
Genetics greatly influence how the body handles cholesterol. A family history of heart attacks, strokes, or high cholesterol can change a patient’s risk level a lot. Kids from families with familial hypercholesterolemia might need cholesterol checks as early as age 2, says the American Academy of Pediatrics.
Underlying Medical Conditions
Certain conditions affect HDL and LDL levels. These include:
- Type 2 diabetes
- Hypothyroidism
- Chronic kidney disease
- Liver disorders
Each condition can raise LDL or lower HDL, making results tricky to interpret. Medications for these conditions can also change lipid values.
Interpreting Results in Conjunction with Other Tests
Doctors look at cholesterol with other risk factors to predict heart disease risk. This guide on blood test codes and health monitoring shows that abnormal results need to be seen in the patient’s full medical context.
| Risk Factor | Impact on Target LDL |
|---|---|
| No risk factors present | Below 130 mg/dL |
| Diabetes or smoking | Below 100 mg/dL |
| Existing heart disease | Below 70 mg/dL |
Understanding cholesterol test fasting needs and reviewing HDL and LDL levels in a broader context helps create personalized treatment plans. These plans go beyond just looking at a lab report.
Limitations of the Test
A lipid panel test is great for checking heart health, but it has its limits. No single test can fully show a person’s heart risk. Knowing these limits helps both patients and doctors make smarter choices.
Variability in Test Results
Cholesterol levels can change daily due to stress, illness, or diet. Even if two people have the same cholesterol reading, their health risks can differ. Doctors often do more tests to get a clear picture before deciding on treatment.
Non-Fasting vs. Fasting Conditions
Most doctors want patients to fast for 9 to 12 hours before the test. They should only drink water during this time. If a patient doesn’t fast right, their triglyceride and LDL levels might look higher than they really are. This can give false results.
Potential for Misinterpretation
Cholesterol test results need a doctor’s expertise to understand. Heart disease is the top killer in the U.S., so getting accurate results is key. The right levels depend on age, family history, lifestyle, and other factors. Without considering these, test results might be misread, causing unnecessary worry or missing important signs for early action.