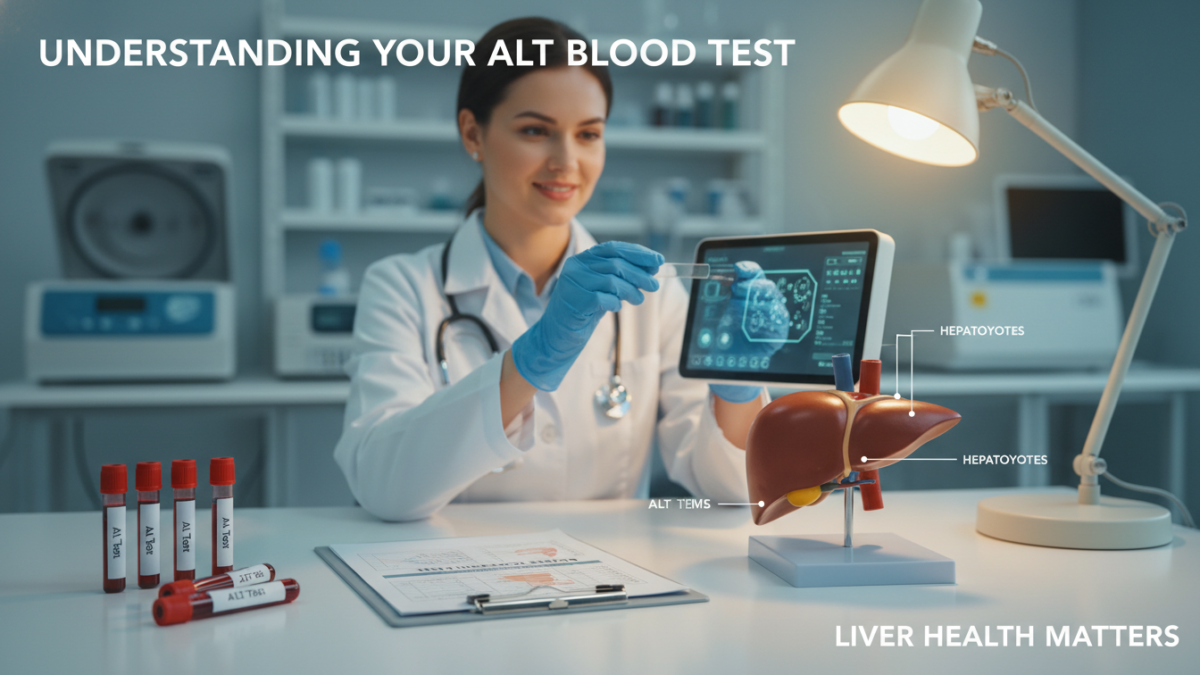
The alanine transaminase assessment (ALT Blood Test) is among the most commonly ordered clinical laboratory examinations for evaluating hepatic health. This measurement provides critical data for diagnosing potential injury or disease.
Alanine transaminase (ALT) is an enzyme found predominantly in hepatic cells. It plays a key role in speeding up specific chemical reactions within the body related to amino acid metabolism.
Under normal conditions, only low concentrations of this enzyme are present in the bloodstream. When liver cells are damaged, they release ALT, leading to elevated levels that can signal hepatic injury.
This analysis is typically performed as part of a standard panel of liver function tests. Understanding the various lab test codes and their purposes is a fundamental aspect of clinical laboratory science.
This article serves as an educational reference for interpreting results. It does not provide medical advice, diagnosis, or treatment recommendations. All decisions regarding personal health should be made in consultation with a licensed healthcare professional.
Key Takeaways
- The ALT assessment is a fundamental diagnostic tool for evaluating liver health and detecting potential abnormalities.
- ALT, or alanine transaminase, is an enzyme primarily located in liver cells and is crucial for metabolism.
- Elevated levels in the bloodstream typically indicate damage or stress to hepatic tissue.
- Interpretation requires knowledge of normal reference ranges and individual clinical context.
- This content is intended as a clinical laboratory reference guide for educational purposes only.
- Personalized interpretation of any laboratory result must come from a qualified healthcare provider.
What the Test Measures
This laboratory analysis quantifies the activity of an enzyme primarily housed within liver cells. It measures the amount of alanine aminotransferase present in the bloodstream.
Understanding Alanine Aminotransferase
This aminotransferase is a protein catalyst found in the cytoplasm of hepatocytes. It consists of 496 amino acids and facilitates a key biochemical transaction.
The enzyme transfers an amino group from L-alanine to alpha-ketoglutarate. This reaction produces L-glutamate and pyruvate.
Enzymes like alanine aminotransferase act as biological catalysts, essential for sustaining life’s chemical reactions in the body.
This process requires pyridoxal phosphate, a form of vitamin B6, as a coenzyme. The table below shows where this transaminase is most concentrated.
| Tissue Type | Relative ALT Concentration | Primary Metabolic Role |
|---|---|---|
| Liver (Hepatocytes) | Very High (≈3000x serum) | Amino acid metabolism, energy production |
| Kidney | Moderate | Amino acid processing |
| Skeletal Muscle | Low | Energy metabolism during exercise |
| Heart (Myocardium) | Low | Cardiac muscle metabolism |
Role in Liver Function and Metabolism
Within hepatic cells, the generated pyruvate enters the tricarboxylic acid (TCA) cycle. This cycle is crucial for cellular energy production.
The aminotransferase integrates into broader liver functions. These include glucose regulation and lipid metabolism.
Under normal conditions, serum levels remain low, typically under 30 IU/L. The enzyme’s circulating half-life is about 47 hours.
Why the Test is Ordered
Measuring this liver enzyme is a standard practice in both preventive health checks and diagnostic evaluations. Clinicians order it to screen for potential issues or to investigate specific concerns.
Routine Blood Screening and Liver Panels
This assessment is often included in a comprehensive metabolic panel during a routine physical. It forms a core part of standard liver function tests.
These panels help establish a baseline for hepatic health. They can detect abnormalities before any physical symptoms appear. This proactive screening is a valuable tool in preventive care.
Assessment of Liver Health and Risk Factors
The test is frequently ordered when a person shows signs of possible liver trouble. Common symptoms include jaundice, abdominal pain or swelling, and unexplained fatigue. Dark urine, light stool, and persistent itching are also indicators.
Individuals with certain risk factors may also undergo this evaluation. These include a history of heavy alcohol use or exposure to hepatitis viruses. The use of specific medications known to affect the liver is another key reason.
Other risk factors involve metabolic conditions like obesity and diabetes. A family history of liver disease can also prompt testing. For those with known hepatic conditions, serial measurements track disease progression or treatment response.
ALT Blood Test Guide: Clinical Context and Reference Ranges
The numerical value from an alanine aminotransferase analysis gains its full meaning only when compared to established clinical benchmarks. These benchmarks, known as reference intervals, provide the essential scale for interpretation.
Normal Reference Range and Units (U/L)
A typical reference interval for this hepatic enzyme is 7 to 56 units per liter (U/L). It is crucial to note that each laboratory defines its own reference range based on its equipment and the population it serves.
Demographic factors significantly influence these ranges. Males generally have higher baseline levels than females. Younger individuals often show higher concentrations than older adults. Ethnicity, such as Mexican American heritage, is also a recognized factor.
The analysis requires a blood sample obtained through a standard venipuncture procedure. This quick process usually takes less than five minutes.
Laboratories use automated analyzers based on photometric principles to measure enzyme activity. For accurate results, specimens must be free of hemolysis, clots, or under-filling.
Alanine aminotransferase levels also follow a daily rhythm, being lowest around 4 AM and highest around 4 PM. A healthcare provider considers all these variables when placing a single measurement into a patient’s unique clinical picture.
What High ALT Levels May Indicate
When test results show concentrations above the normal range, healthcare providers consider various potential causes. Elevated readings often serve as clues to underlying hepatic issues.
Potential Liver Cell Injury and Damage
Higher-than-usual enzyme activity typically suggests hepatocyte membrane compromise. This cellular injury releases the enzyme into circulation at measurable levels.
Specific patterns emerge with different causes. Alcohol consumption can lead to hepatic stress with variable elevation. Drug-induced injury, particularly from certain pain relievers, frequently produces dramatic increases.
Ischemic events from reduced blood flow create rapid, marked elevations. These situations require prompt clinical assessment to determine the exact source of hepatic distress.
Associations with Liver Diseases
Non-alcoholic fatty liver disease represents a common metabolic association. This condition correlates with obesity and insulin resistance patterns.
Viral infections, including hepatitis strains, produce characteristic elevation profiles. Autoimmune disorders and genetic conditions like hemochromatosis may also present with chronic increases.
Cirrhosis and hepatic malignancies show variable patterns. Advanced scarring might paradoxically show only mild elevation despite significant disease progression.
All findings must be interpreted within a complete clinical picture. Only qualified professionals can determine what specific patterns mean for individual health situations.
What Low ALT Levels May Indicate
While elevated enzyme activity often signals concern, lower-than-expected levels present a different clinical picture. Findings below the standard reference range for alanine aminotransferase are uncommon. They generally receive less clinical attention than high readings.
Reduced concentrations are not typically linked to acute liver problems. Healthcare providers view them within the broader context of a patient’s health.
Possible Link to Vitamin B6 Deficiency or Other Factors
A notably low level may be associated with a vitamin B6 deficiency. This vitamin, as pyridoxal 5′-phosphate, acts as a necessary coenzyme for the hepatic enzyme’s function.
Without adequate B6, the enzyme’s catalytic activity in transamination reactions can decrease. This can lead to a lower measured concentration in the bloodstream.
Some studies link chronic kidney disease to lower alanine aminotransferase levels. The exact mechanism and importance of this association are still being researched.
An isolated low finding often prompts a repeat analysis. This step confirms the result and rules out lab errors or specimen issues.
The clinical meaning of a mildly reduced level is often uncertain. Providers interpret it alongside other lab parameters and the patient’s overall presentation.
| Factor | Proposed Mechanism | Clinical Consideration |
|---|---|---|
| Vitamin B6 Deficiency | Insufficient coenzyme (pyridoxal 5′-phosphate) for catalytic activity | May warrant nutritional assessment; often reversible with supplementation |
| Chronic Kidney Disease | Altered metabolism or clearance; association not fully understood | Correlation observed; significance in disease monitoring is unclear |
| Isolated Low Finding | Pre-analytical error, lab variability, or biological individuality | Typically requires confirmation with repeat testing before further action |
Related Biomarkers and Complementary Tests
The interpretation of alanine aminotransferase levels is frequently enhanced by comparing them with other related enzymes. This enzyme is rarely assessed in isolation within clinical practice.
It is typically part of a standard liver function panel. This panel includes several key indicators that provide a more complete picture of hepatic health.
Comparison with AST and Other Liver Enzymes
Aspartate transaminase (AST) is measured concurrently with alanine aminotransferase. Both are transaminase enzymes released during liver cell injury.
However, AST is found in many tissues like heart and muscle. This makes the alanine enzyme more specific for hepatic issues.

The AST-to-ALT ratio helps clinicians determine the cause of damage. A high ratio often points to alcoholic liver disease, while a low ratio suggests other conditions.
Additional Liver Function Indicators
Other enzymes like alkaline phosphatase (ALP) and gamma-glutamyltransferase (GGT) are also checked. They indicate problems with bile flow or cholestasis.
Tests measuring bilirubin, albumin, and prothrombin time assess the liver’s synthetic function. These results show how well the organ is working, not just if it is injured.
Further tests may include viral hepatitis screens and metabolic markers. A comprehensive approach helps identify the precise reason for any enzyme elevation.
Factors That Affect ALT Results
The measured value of this hepatic enzyme is not static and can be modified by a range of demographic and lifestyle factors. These variables must be considered to avoid misinterpreting a single measurement.
Influence of Medications, Diet, and Exercise
Many pharmaceutical agents can influence alanine aminotransferase concentrations. Common medications include certain pain relievers, antibiotics like amoxicillin-clavulanate, and statins.
Intense physical exertion can cause a temporary, reversible increase. This elevation likely comes from muscle tissue, not the liver.
Fasting status may be requested if the enzyme is part of a larger metabolic panel. Diet itself does not directly change the enzyme level.
Impact of Age, Gender, and Ethnicity
Biological sex is a key demographic factor. Males typically have higher baseline concentrations than females.
Age also plays a role. Younger individuals often show higher levels than older adults. Ethnic background, such as Mexican American heritage, is associated with different reference ranges.
Body mass index is a major determinant. Higher BMI, often linked to non-alcoholic fatty liver disease, correlates with elevated readings.
Other physiological rhythms matter. Levels follow a daily pattern, lowest around 4 AM and peaking near 4 PM. For women, menstrual cycle phase can contribute to normal variation.
| Factor | Typical Effect | Clinical Note |
|---|---|---|
| Intense Exercise | Temporary Increase (~2x) | Resolves with rest; origin is skeletal muscle |
| Common Medications | Variable Increase | Includes analgesics, antibiotics, statins, anticonvulsants |
| Biological Sex | Higher in Males | Related to hormones and body composition |
| Body Mass Index (High) | Often Elevated | Strongly associated with metabolic conditions |
When Clinical Evaluation is Recommended
In clinical practice, the decision to pursue additional evaluation hinges on the pattern and context of liver enzyme elevations. A single abnormal result is often not definitive.
Indicators for Further Medical Assessment
Marked elevations, especially levels exceeding 1000 U/L, typically prompt investigation. Persistence of high readings for more than six months may indicate a chronic condition.
Concurrent symptoms like jaundice, abdominal pain, or severe fatigue also signal a need for assessment. In acute viral hepatitis, enzyme levels usually peak between days 7 and 12.

Levels normally return to baseline within three to five weeks if recovery is straightforward. The table below outlines common clinical triggers.
| Clinical Indicator | Typical Threshold | Associated Concern |
|---|---|---|
| Enzyme Elevation | >1000 U/L | Acute hepatocellular injury |
| Duration of Elevation | >6 months | Chronic hepatitis or disease |
| Symptom Presence | Jaundice, Ascites | Advanced hepatic dysfunction |
Integrating Risk Factors with Lab Findings
A thorough patient history is crucial. It reviews medication use, alcohol intake, and family history of genetic liver disorders.
Metabolic risk factors like obesity and diabetes are integrated with the test results. Physical exam findings such as ascites or peripheral edema add important context.
It is noted that a significant portion of patients with chronic hepatitis C can have persistently normal readings. This highlights why risk factor integration is essential for a complete clinical picture.
Conclusion
The journey from a lab report to a clear health picture involves careful professional interpretation. This resource has detailed how a common hepatic enzyme serves as a sensitive marker for liver cell status.
While an ALT blood test is a valuable tool, its results are not a diagnosis. Healthcare providers consider these findings alongside symptoms, history, and other tests.
Many factors influence enzyme levels, and not every high reading indicates a serious problem. Persistent changes or concerning patterns warrant a deeper look.
This guide offers evidence-based information to support your health literacy. Always consult a qualified provider for personalized medical advice and interpretation of any lab result.