The liver function test is a common test in healthcare. It checks the liver’s health by looking at substances like ALT, AST, and bilirubin. Doctors use these tests to find diseases, track treatments, and make care plans.
The liver is in the right upper abdomen and does many important jobs. It breaks down toxins, makes proteins, and helps with digestion. If the liver can’t do these jobs well, a liver test can show problems early.
About 8% of people have high liver test values. But, up to 30% of these values go back to normal in three weeks without treatment. If a test shows something’s wrong, doctors use the R ratio to figure out the type of damage.
Understanding liver tests is key for both patients and doctors. Tests like PT and INR show how well the liver works. These tests give a complete picture of the liver’s health.
Key Takeaways
- Liver function tests measure enzymes, proteins, and bilirubin to evaluate liver health and detect damage early.
- The liver performs critical roles including detoxification, protein synthesis, bile production, and glucose regulation.
- Roughly 8% of people tested show elevated LFT values, and about 30% of those normalize within three weeks.
- The R ratio formula helps classify liver injury as hepatocellular, cholestatic, or mixed based on enzyme levels.
- Prothrombin time and INR are included to assess the liver’s ability to produce clotting factors.
- Accurate liver function test interpretation requires clinical context, not just isolated lab numbers.
What the Test Measures
A liver function test (LFT) checks several markers to see how well the liver works. Knowing what each marker means is key. A full test looks at enzymes, bilirubin, and proteins, each telling a part of the liver’s story.
Key Liver Enzymes
Alanine aminotransferase (ALT) is mostly found in liver cells. It has a half-life of about 47 hours and is very liver-specific. Aspartate aminotransferase (AST) is in the liver, heart, muscles, kidneys, and brain. High levels of ALT and AST often mean liver cell damage or inflammation.
Two other enzymes are also tested:
- Alkaline phosphatase (ALP) — found in bile duct walls, bone, and intestines
- Gamma-glutamyl transferase (GGT) — present in the kidneys, pancreas, and liver
| Enzyme | Primary Source | Clinical Significance |
|---|---|---|
| ALT | Liver (cytoplasm) | Most specific for liver damage |
| AST | Liver, heart, muscle | Indicates broader tissue injury |
| ALP | Bile ducts, bone | Suggests bile flow obstruction |
| GGT | Liver, kidneys, pancreas | Confirms biliary or alcohol-related issues |
Bilirubin Levels
About 80% of bilirubin comes from breaking down hemoglobin in old red blood cells. The unconjugated form goes to the liver bound to albumin. There, it’s changed into a conjugated form for bile excretion. High bilirubin can cause jaundice and show liver processing problems.
Protein Production Markers
Albumin is made by liver cells and lasts about 21 days. Even with just 10% of liver cells working, the liver can keep albumin levels normal. Total protein includes albumin and globulins. Low levels can mean chronic liver problems, which we’ll explore next.
Why It Is Ordered
Doctors order liver function tests for many reasons. They are part of routine checkups or targeted tests. These tests help find problems early. A common test, the comprehensive metabolic panel (CMP), checks liver health.
Assessing Liver Health
Routine tests catch liver problems early. Doctors look at enzyme levels to find out what’s wrong. This helps them understand the problem better.
People at high risk, like those with obesity or diabetes, need regular tests. Even if they feel okay.
Investigating Symptoms
Some symptoms make doctors order these tests right away. They look at the patient’s symptoms and test results together. This helps them understand the situation better.
- Jaundice (yellowing of the skin and eyes)
- Persistent nausea, vomiting, or loss of appetite
- Unexplained fatigue and weakness
- Dark urine or light-colored stool
- Abdominal pain, swelling, or leg edema
Early detection through blood work remains one of the most effective tools in preventing irreversible liver damage.
Monitoring Liver Conditions
For those with liver diseases, tests track how the disease is progressing. They see if treatments are working. This helps doctors make changes to treatment plans.
This monitoring is key to making the right decisions. It’s based on specific numbers.
Normal Reference Range
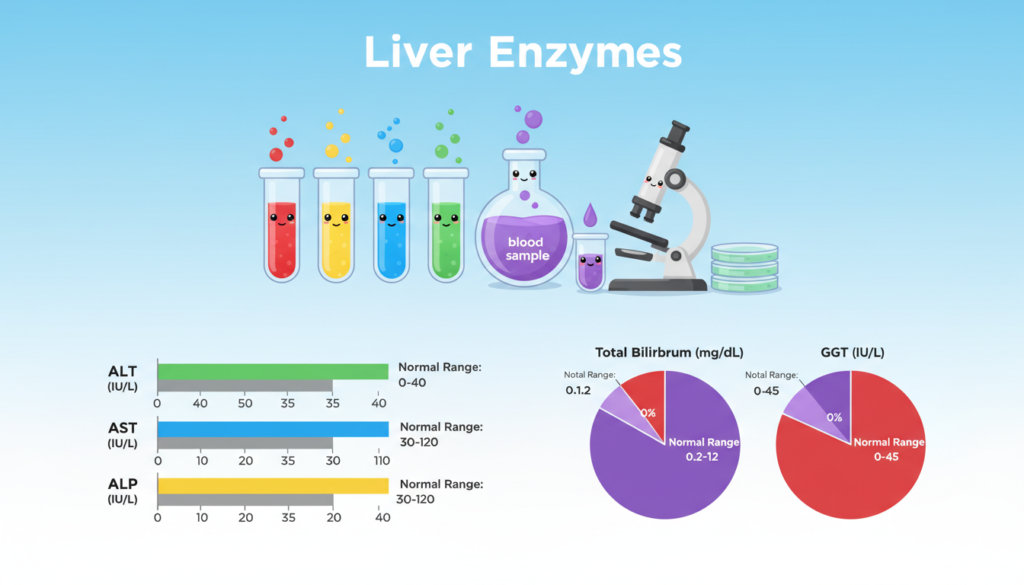
Understanding the normal ranges for liver tests is key. These ranges help doctors understand what abnormal liver enzyme levels mean. These values can change based on age, sex, body mass index (BMI), and blood type.
Males tend to show higher enzyme values than females. People with a BMI over 30 kg/m² might have 40–50% higher ALT values and 50% higher GGT readings. Regular exercise can lower ALT levels by about 20%.
Enzyme Levels (units: U/L)
Elevated ALT and AST levels are common concerns on liver tests. Here are the typical healthy ranges:
| Enzyme | Normal Range (U/L) | Key Notes |
|---|---|---|
| ALT (Alanine Aminotransferase) | 3–30 | Higher in males; rises with elevated BMI |
| AST (Aspartate Aminotransferase) | 11–32 | Found in liver, heart, and muscle tissue |
| ALP (Alkaline Phosphatase) | 35–150 | Can rise after food intake in blood groups B and O |
| GGT (Gamma-Glutamyl Transferase) | 5–40 | Sensitive to alcohol use; plateaus around age 50 |
Food can cause ALP to increase by up to 30 U/L. This increase can last for 12 hours.
Bilirubin Levels (units: mg/dL)
Interpreting bilirubin levels is important. The standard total bilirubin range is 0.3–1.1 mg/dL. Levels above this might indicate bile duct problems or red blood cell breakdown issues.
Protein Levels (units: g/dL)
Albumin and total protein show how well the liver makes proteins. These levels can change due to:
- Dietary protein intake
- Hydration status
- Colloidal osmotic pressure changes
A drop in albumin below the expected range often signals chronic liver stress or poor nutrition. Doctors look at enzyme and bilirubin findings along with protein levels for a full picture.
What High Levels May Indicate
When liver function tests show high levels, it means the liver is under stress. Doctors use these tests to find out if the problem is with liver cells or bile flow. Each issue needs a different treatment.
Liver Damage or Disease
Liver injury is shown when ALT is more than three times normal or bilirubin is over twice normal. High AST or ALT levels, over ten times normal, often mean toxin exposure or poor blood flow. Taking too much acetaminophen, certain antidepressants, and anticonvulsants can also cause liver enzyme spikes.
Nonalcoholic steatohepatitis (NASH) affects up to 5% of Americans. In these cases, liver enzyme levels are usually below four times normal. It’s important to know about alkaline phosphatase high causes, as conditions like sarcoidosis, metastatic cancer, and lymphoma can show a cholestatic pattern.
Bile Duct Obstruction
High ALP levels, over twice normal, with high bilirubin suggest blocked bile ducts. Primary sclerosing cholangitis and primary biliary cirrhosis are common causes. Imaging studies are needed to confirm these cholestatic conditions.
Alcohol-Related Liver Damage
The GGT test is key when alcohol use is suspected. An AST-to-ALT ratio of 2:1 with high GGT points to alcoholic liver disease in over 90% of cases. This number goes up to 96% with a ratio of 3:1.
| Pattern | Key Marker Elevation | Likely Condition |
|---|---|---|
| Hepatocellular | ALT/AST > 3× normal | Viral hepatitis, drug toxicity, NASH |
| Cholestatic | ALP > 2× normal + high bilirubin | Bile duct obstruction, biliary cirrhosis |
| Alcoholic | AST:ALT ratio ≥ 2:1, elevated GGT | Alcoholic liver disease |
What Low Levels May Indicate
Low values on a liver panel can be just as important as high ones. It’s key to understand what low levels mean. Low albumin, total protein, or enzyme levels can signal serious health issues.
Liver Dysfunction
The liver makes albumin and clotting factors. If it can’t keep up, albumin levels drop. Even with just 10% of its cells, the liver can synthesize enough albumin.
But, if damage goes beyond 10%, albumin levels start to fall. This is a sign of liver trouble.
Low vitamin K-dependent clotting factors are another warning sign. Prolonged clotting times and low protein levels point to liver issues.
Malnutrition
Low albumin doesn’t always mean liver disease. Poor diet, malabsorption, and other conditions can also lower albumin levels. It’s important to know the difference between nutritional and liver-related causes.
A person with a normal liver but a bad diet can have the same low albumin as someone with liver disease.
Chronic Liver Disease
Diseases like cirrhosis, primary biliary cholangitis, and hemochromatosis damage the liver over time. As the liver gets scarred, it can’t make enough protein.
Even with normal enzyme levels, hepatitis C and nonalcoholic steatohepatitis can cause liver damage. Research in the American Journal of Gastroenterology shows this.
| Condition | Albumin Level | Clotting Factor Production | Enzyme Levels |
|---|---|---|---|
| Early Cirrhosis | Low-normal | Mildly reduced | May be normal |
| Advanced Cirrhosis | Significantly low | Markedly reduced | Variable |
| Malnutrition | Low | Normal | Normal |
| Nephrotic Syndrome | Low (protein loss) | Normal | Normal |
Understanding liver function tests requires looking at the whole picture. It’s not just about one value on a lab report.
Related Biomarkers

Liver function tests are often used with other blood tests. This helps doctors understand a patient’s health better. By looking at several biomarkers together, doctors can find the cause of liver enzyme problems.
Complete Blood Count (CBC)
A CBC shows important information about blood cells. It can reveal issues like portal hypertension or cirrhosis. It also helps find infections or inflammation in the liver.
Prothrombin Time (PT)
PT checks how fast blood clots. The liver makes clotting factors that PT measures. If the liver is damaged, clotting slows, and PT goes up.
Hepatitis Panel
Screening for hepatitis B includes several tests. A positive surface antigen with a positive core antibody means active infection. Hepatitis C antibody tests are for those who have used IV drugs.
Specialized markers add more to the evaluation:
- Alpha-fetoprotein (AFP) — detects liver cancer
- Carbohydrate-deficient transferrin (CDT) — shows alcohol intake
- CA19-9 — tracks primary sclerosing cholangitis
- Serum ferritin — checks for hemochromatosis
| Biomarker | Primary Purpose | Key Clinical Insight |
|---|---|---|
| CBC | Blood cell evaluation | Low platelets suggest cirrhosis |
| Prothrombin Time | Clotting ability | Prolonged PT reflects impaired liver synthesis |
| Hepatitis B Panel | Viral infection screening | Surface antigen confirms active infection |
| Hepatitis C Antibody | Viral infection screening | Positive result requires confirmatory RNA test |
| Alpha-fetoprotein | Tumor marker | Elevated in hepatocellular malignancies |
| Serum Ferritin | Iron storage assessment | High levels may indicate hemochromatosis |
Factors That Affect Results
Understanding liver enzyme test results is more than just looking at numbers. Many outside factors can change the results and make them hard to understand. It’s important to think about what might have affected the readings before making conclusions.
Medications and Supplements
Drug-induced liver injury happens in about 19 cases per 100,000 people each year. Amoxicillin-clavulanate is the most common cause. Drugs like bupropion, fluoxetine, sertraline, and valproic acid can also cause liver damage, leading to high ALT and AST levels.
Other drugs can cause different types of liver injury:
| Injury Pattern | Common Medications |
|---|---|
| Hepatocellular | Bupropion, Fluoxetine, Risperidone, Valproic Acid |
| Cholestatic | Chlorpromazine, Mirtazapine, Tricyclic Antidepressants |
| Mixed | Carbamazepine, Phenytoin, Amitriptyline, Phenobarbital |
Herbal remedies like germander and kava can also affect test results. Metronidazole can interfere with ALT measurements because of its absorbance near 340 nm.
Diet and Nutrition
Getting accurate liver test results depends on timing and sample quality. ALT levels can change by up to 45% throughout the day, with higher values in the afternoon. A high-fat meal can also distort colorimetric assays due to light scattering.
Fasting before blood draws helps reduce interference from dietary factors, improving the reliability of liver enzyme measurements.
Recent Illness or Injury
Acute infections and physical trauma can temporarily change enzyme readings. A condition called benign transient hyperphosphatasemia can cause ALP levels to spike into the thousands of IU/L. It often appears with infections and returns to normal in 6–8 weeks.
Hemolysis from blood sample handling can also skew results at specific wavelengths. This makes understanding liver enzyme results even more complex. It shows why looking at related biomarkers and clinical context is so important for accurate diagnosis.
Clinical Context Considerations
Lab numbers alone never tell the full story. A proper liver panel understanding demands that clinicians weigh test values against each patient’s unique clinical picture. Symptoms, physical exam findings, lifestyle factors, and imaging all shape how LFT results explained by a provider translate into a diagnosis or treatment plan.
Patient History
A thorough medical history is the foundation of hepatic function markers analysis. Clinicians should review all medications — prescription, over-the-counter, and herbal supplements. Substances like acetaminophen, statins, and certain herbal therapies can elevate liver enzymes on their own.
The history should capture:
- Alcohol intake and recreational drug use (including MDMA, phencyclidine, or inhaled solvents)
- Prior blood transfusions or organ transplants
- Family history of liver disease
- Signs of chronic liver disease on exam — jaundice, ascites, palmar erythema, or temporal wasting
Risk Factors for Liver Disease
Specific conditions require targeted screening when abnormal results appear. The following conditions illustrate how liver panel understanding guides deeper investigation:
| Condition | Key Clue | Confirmatory Test |
|---|---|---|
| Hemochromatosis | Transferrin saturation >45% | HFE gene mutation analysis |
| Autoimmune Hepatitis | Women ages 20–50; hypergammaglobulinemia in >80% | ANA, anti-smooth muscle antibodies |
| Wilson Disease | Low ceruloplasmin; tremor, rigidity, slurred speech | 24-hour urine copper |
| Celiac Disease | Chronic diarrhea, abdominal distension | Tissue transglutaminase and anti-endomysial antibodies |
IV drug use, tattoos, and occupational blood exposure raise risk for viral hepatitis and should prompt serologic testing.
Correlation with Imaging Studies
When LFT results explained by lab work suggest bile duct obstruction or structural disease, right upper quadrant ultrasonography is the standard first-line imaging study. It can detect gallstones, partial bile duct blockage, fatty infiltration, and liver masses — giving clinicians the visual context that hepatic function markers analysis requires for accurate decision-making.
Limitations of the Test
A liver function test is useful but has its limits. Many say it’s misleading because it shows liver damage, not function. Only albumin and prothrombin time show how well the liver makes proteins. It’s important to understand this to get the right picture.
Variability in Results
Test results can change due to how the sample is handled and the lab conditions. Samples must be processed quickly and kept cold for up to eight hours. If testing takes longer than 48 hours, they should be frozen.
Photometry-based analyzers use a specific law, and small changes in the sample can affect the results. For example, bilirubin levels can change if the sample is exposed to light or delayed.
Not a Complete Diagnosis
Even normal test results don’t mean there’s no serious disease. Up to 16% of hepatitis C patients and about 13% with nonalcoholic steatohepatitis can have normal lab results but have liver damage. High alkaline phosphatase levels can mean cholestatic injury, but a mix of high levels needs careful analysis.
Isolated high bilirubin levels with normal enzymes suggest a different problem. This means more tests are needed to find the cause.
Importance of Follow-up Testing
Patients with normal results but high levels should have tests repeated. If the second test is normal, a third test in three to six months is advised. By looking at all the test results together, doctors can better understand liver problems.
No single test can tell the whole story. That’s why follow-up tests are key for accurate diagnosis and treatment.



